
This post, which mostly provides useful citations, was originally written as an answer to the following Quora question:
Is ADHD one of the only psychiatric conditions that can be diagnosed objectively?

This post, which mostly provides useful citations, was originally written as an answer to the following Quora question:
Is ADHD one of the only psychiatric conditions that can be diagnosed objectively?
I am currently reading an excellent paper that will be published in Behavioral and Brain Sciences soon. It raises some very important issues with popular conceptions of mental illness.
Brain disorders? Not really… Why network structures block reductionism in psychopathology research
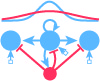
These two figures capture some of the key points:
Here is the abstract:
“In the past decades, reductionism has dominated both research directions and funding policies in clinical psychology and psychiatry. However, the intense search for the biological basis of mental disorders has not resulted in conclusive reductionist explanations of psychopathology. Recently, network models have been proposed as an alternative framework for the analysis of mental disorders, in which mental disorders arise from the causal interplay between symptoms. In this paper, we show that this conceptualization can help understand why reductionist approaches in psychiatry and clinical psychology are on the wrong track. First, symptom networks preclude the identification of a common cause of symptomatology with a neurobiological condition, because in symptom networks there is no such common cause. Second, symptom network relations depend on the content of mental states and as such feature intentionality. Third, the strength of network relations is highly likely to partially depend on cultural and historical contexts as well as external mechanisms in the environment. Taken together, these properties suggest that, if mental disorders are indeed networks of causally related symptoms, reductionist accounts cannot achieve the level of success associated with reductionist disease models in modern medicine. As an alternative strategy, we propose to interpret network structures in terms of D. C. Dennett’s (1987) notion of real patterns, and suggest that, instead of being reducible to a biological basis, mental disorders feature biological and psychological factors that are deeply intertwined in feedback loops. This suggests that neither psychological nor biological levels can claim causal or explanatory priority, and that a holistic research strategy is necessary for progress in the study of mental disorders.”
Behavioral and Brain Sciences is one of the premier journals for “big thinking” in cognitive science and neuroscience, so it’s great to see these ideas there.